Sleep Apnea & Snoring
Obstructive sleep apnea is a serious medical condition in which the soft tissues at the back of the throat completely close off the airway so that air cannot flow into the lungs. This airway blockage can reduce the amount of oxygen reaching the brain and body. When that happens, the brain alerts the muscles in the airway to tighten up and unblock the air passage. As the air starts to flow into the lungs again, a loud gasp or snort (sometimes called a ‘resuscitative snort’) is heard. The patient may also sit up or move violently before falling back into a light sleep. Bruxism or Teeth Grinding is also a compensatory mechanism which the body uses to try to keep the airway open. This excessive grinding can cause temporomandibular joint disease.Then breathing (and frequently snoring) begins again. This process of blocking and unblocking the airway causes a significant and very negative disruption of sleep patterns.
Snoring
Snoring can be a real problem, not only for the person who snores, but for the partner and other family members who live with the snorer. However, there is a dentist-prescribed solution for a more restful night’s sleep: Silent Nite. This device is flexible, thin and comfortable for patients, and it exhibits documented clinical success in mitigating or even preventing the disruptive, unhealthy effects of snoring and sleep apnea.
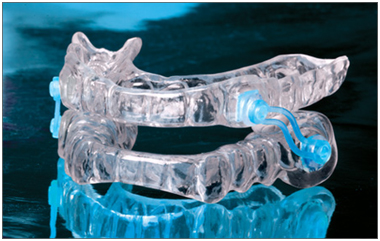
Silent Nite positions the lower jaw forward using special S-shaped connectors that are attached to upper and lower trays. These trays are comprised of a soft inner layer with a hard outer layer that is durable and BPA-free.
TMD – Temporomandibular disorder
The jaw joints and groups of muscles that let us chew, swallow, speak and yawn are known as the temporomandibular. When there’s a problem with how the joints and muscles work, you may have a temporomandibular disorder or TMD.
Symptoms
The symptoms of TMDs are:
- Tender or sore jaw muscles. Your jaw may be even more painful when you wake up, clench your teeth, chew your food or yawn.
- Problems opening or closing your mouth. It may be hard to open or close your jaws all the way, or your jaws may lock open or closed.
- Headaches that you cannot explain. You may also feel pain in your neck. These may be caused by TMD, or by other problems. Tell your dentist AND your doctor.
- A clicking or grinding noise when you chew or yawn. You may hear strange noises in your jaw joints, such as clicking or popping when you open your mouth, or crunching and grinding sounds when you chew.
Cause and Effect
The cause of TMD is not always clear, but in most cases stress is a major factor. Here are some of the things that MAY cause it:
- Clenching and grinding your teeth. Clenching your jaw muscles can cause them to ache. Some people grind their teeth or clench their jaw muscles when they are under stress.
- Injury to your face or jaws. Broken (or fractured) jaws, a jaw joint that has been knocked out of place (or dislocated) and “whiplash” may cause TMD.
- Some diseases, such as rheumatoid arthritis, may affect the jaw joints and muscles.
- If your jaw does not grow the right way, your teeth may not line up the way they should. This can make it hard to bite and chew, and may lead to TMD.
Other things that MAY leads to TMD are:
- worn, loose, or missing teeth
- gum problems
- partial or full dentures that are not the right fit
- habits such as biting on your pen or pencil
What you can do
1. Relax. Be aware of when you are clenching your teeth. Try to relax your jaw muscles and keep them relaxed. If you need help learning to relax, there are courses that can teach you. Ask your dentist or doctor.
2. Watch what you eat. Stay away from hard or sticky foods. Do not chew gum. Eat a soft diet and cut food into small pieces. Try not to open your mouth too wide, even when you yawn.
3. Massage and exercise. Rub (or massage) and stretch (or exercise) your jaw muscles. This may help ease stress, just like it does with other muscles in your body. But be gentle. Too much stretching or exercising could make the problem worse.
4. Use a compress. Your dentist may suggest putting a cold or warm compress on your sore jaw muscles, then rubbing (or massaging) them gently to help ease tense muscles. For a cold compress, use ice cubes wrapped in a towel, or a bag of frozen vegetables such as peas. For a warm compress, use a hot water bottle or heating pad wrapped in a towel, or a hot, damp cloth.
5. Remember the saying, “Lips together … teeth apart.” When you are relaxed:
- your teeth should be slightly apart,
- your tongue should be resting gently against the roof of your mouth and
- Your lips should be relaxed and barely touching or slightly apart.
Try to keep your upper and lower teeth apart, except when you are eating or swallowing.
6. Think positively. Almost all TMD patients get better, but there is no “easy cure.” For some patients, once they know that they clench their jaws, they make an effort to relax. They can ease their symptoms in a few days or weeks. For others, it may take several weeks or several months before they feel better.
How your dentist can help
To judge your condition, your dentist:
- will do a detailed exam, and
- may take x-rays.
Depending on what your dentist finds, he or she may suggest a plan to treat your TMD. Your dentist may also refer you to a dental specialist with extra training in TMDs. This could be an oral surgeon (also called an oral and maxillofacial surgeon), an oral pathologist, an orthodontist, a periodontist or a prosthodontist. If your dentist refers you to a dental specialist, he or she will explain what that specialist does.
Treatment may include:
- Referring you to another health care worker to help you ease muscle pain or open your jaw. This could be a physiotherapist, a chiropractor and/or a behavioral therapist.
- Correcting problems with your teeth. If you have a bad bite, braces or other dental work may be used to correct the problem. Teeth that are causing the problem can sometimes be reshaped to fit together better.
- Taking medicine. Depending on the cause of your TMD, medicine for pain, inflammation, tense muscles or depression may help.
- Wearing a night guard or bite plate (also called an occlusal splint). An occlusal splint is made of clear plastic. It fits over the biting surface of the teeth of one jaw so that you bite against the splint rather than your teeth. This helps your jaw joints and muscles to relax. Depending on your TMD, your dentist may tell you to wear a splint 24 hours a day, only at night, or for some length of time in between.
- Having surgery. If none of the other treatments have worked, or if it is VERY hard to open your jaw, you MAY need surgery.
Nutrition
If you want to maintain strong teeth for your lifetime, you need to ensure you are eating enough whole grain breads and cereals, fruits and vegetables and lean meats.
Some other healthy snack choices include:
- nuts and seeds
- peanut butter
- cheese
- plain yogurt
- popcorn
Acid Erosion
There are some drinks and snacks that are bad for your teeth and may contribute to acid erosion. Acid erosion happens when food or drink with a low PH level (more acidic) are consumed. That acid can linger in your mouth, taking the minerals away and softening the surface of your teeth. This makes your teeth more susceptible to damage and often leads to increased sensitivity and may require treatment. The big offenders seem to be soft drinks, orange juice and lemonade.
Nutrition Tips
- Try to avoid acidic food and drink between meals; there isn’t as much saliva in your mouth at these times to protect your teeth
- Don’t clean your teeth right after eating. If you brush while the acid is still in your mouth you are removing some of your teeth’s surface. If you wait about an hour the saliva will help your teeth battle the acid so it is safe to brush
- Try to finish your breakfast, lunch or dinner with a little cheese or milk as these products help cut down on the acid in your mouth.
A Note about Sweets
When it comes to your teeth, it’s not about the amount of sweets you eat, but the length of time that you leave your teeth exposed to sweets. So it’s better to eat sweets at mealtimes rather than between meals, as the amount of saliva produced at mealtimes will help protect your teeth.
If you cannot avoid sweets between meals, choose something with less sugar like those listed above. Sticky sweets like toffee or hard candy should be avoided as snacks.
Pregnancy & Early Childhood Development
Keeping your teeth and gums healthy during pregnancy has many benefits for you and your baby.
Your body undergoes many changes during pregnancy. Some of these can affect the health of your gums and teeth.
- Changes in your hormone levels can cause swollen gums that bleed during cleaning (pregnancy gingivitis).
- The risk of having a premature or low birth-weight baby may be reduced if you have healthy gums and teeth.
- Morning sickness can leave stomach acids in your mouth. These acids can damage the surface of the teeth and promote tooth decay.
You can help yourself
Taking care of your oral health is always a good idea. While pregnant, there are particular things you can do to help.
- Keep your mouth clean. Brush twice each day using a fluoride toothpaste
- Floss daily to remove plaque from between your teeth and gums.
- Eat healthy, nutritious food.
- Try eating dry toast or unsalted crackers before getting out of bed in the morning to help prevent morning sickness.
- If you do vomit, rinse your mouth with water or a fluoride mouth rinse. Rinsing helps protect your teeth from damaging stomach acids.
- If you have any questions about your oral health, ask your dentist or hygienist.
Dentists provide special care to pregnant women
Your dentist and dental hygienist have special training to look after your oral health while you are pregnant. It is best to arrange a visit in the middle three months of your pregnancy.
- Tell your dentist that you are pregnant.
- Regular dental cleanings and check-ups before, during and after your pregnancy are important.
- Put off routine x-rays until after your pregnancy.
- If your dentist recommends dental x-rays, the dental office will provide a leaded apron to shield you and your baby from the low dose of radiation used.
- Avoid taking drugs or medications while pregnant. If emergency dental treatment requires that you take drugs, be sure to discuss their use with your dentist and physician.
Oral Cancer
The Canadian Cancer Society estimates that 3,400 new cases of oral cancer were diagnosed in Canada in 2010. It is also estimated that 1,150 of those Canadians diagnosed in 2010 will die from the disease.1
This too-often fatal condition has a greater mortality rate than both breast cancer and prostate cancer. However, oral cancer can be successfully treated if caught at an early stage.
Your dentist can play an important role in the early detection of oral cancer. Dentistry is about prevention and the dental exam is the foundation of good oral health. A dentist may notice subtle changes in the mouth that a patient won’t.
The oral cancer examination performed by your dentist during a routine dental exam is fast, easy and painless – and it could save your life.
Book your dental exam today – your health will thank you for it!
What is oral cancer?
Oral cancer refers to all cancers of the oral cavity, which includes the following:
- lips
- tongue
- teeth
- gums (gingiva)
- lining inside the lips and cheeks (labial mucosa and buccal mucosa)
- floor of the mouth
- roof of the mouth (palate)
- the area behind the wisdom teeth
Most oral cancers are located on the sides of the tongue, floor of the mouth and lips. Oral cancer starts in the cells of the mouth. Normally these cells are quite resistant to damage, but repeated injury from smoking, alcohol or even friction may cause sores or painful areas where cancer can start.
Symptoms
Oral cancer symptoms include:
- a sore on the lip or in the mouth that does not heal
- a lump on the lip or in the mouth or throat
- a white or red patch on the gums, tongue or lining of the mouth
- unusual bleeding, pain or numbness in the mouth
- a sore throat that does not go away, or a feeling that something is caught in the throat
- difficulty or pain with chewing or swallowing
- swelling of the jaw that causes dentures to fit poorly or become uncomfortable
- a change in the voice and/or pain in the ear
Your Dental Exam
Your dentist does more than protect and care for your teeth, gums and smile — your dentist can also help keep you healthy.
As oral health experts, dentists are in a unique position to help in the early detection of many medical conditions, including cancer.
Dentists are trained in medicine so they recognize the relationships between oral and overall health.
Most people see their dentist regularly, so your dentist is often the first health-care professional to have an opportunity to detect the many health conditions that affect your mouth. Many patients are not aware of the extent that a dental exam can play in disease prevention.
Through the dental exam, your dentist can see if there are any abnormalities or changes in your mouth that might be indications of health problems, such as oral cancer or diabetes. At each visit, your dentist will conduct a medical history review and ask you about your current health.
It’s important to answer these questions carefully. What you say can help your dentist alert you to potential health concerns that may require further investigation, diagnosis or treatment by a physician.
Without an examination by a dentist, most early signs of oral cancer are difficult to detect. If you notice a mouth sore or anything out of the ordinary that does not go away or heal after a couple of weeks, discuss it with your dentist.
Risk Factors
- Smoking and chewing tobacco — particularly if combined with heavy alcohol consumption
- Heavy alcohol consumption — particularly if combined with smoking
- Excessive sun exposure — particularly to the lip
- Age — people over the age of 40 have a higher risk of developing oral cancer
- Gender — men are more susceptible than women to developing oral cancer. In the past, men had a 6:1 ratio of incidence of oral cancer compared to women. However; this ratio is narrowing and is now closer to a 2:1 ratio
- HPV — more research is emerging that connects human papillomavirus infection — especially HPV-16 — with oral cancers
- A diet low in fruits and vegetables — fruit and vegetables have a protective factor that is believed to reduce the risk for oral cancers
Prevention
- See a dental professional for a regular dental exam
- Quitting (or reducing) your tobacco and alcohol use lowers your risk of developing oral cancer
- When you are outside and exposed to the sun, use lip balm with UV protection and wear a hat
- Eat a healthy diet rich in fruits and vegetables
- Brush and floss your teeth daily
The mouth has long been recognized as a mirror reflecting the health of the body. With regular visits to your dentist and good oral health routines, you will have lots to smile about.
Smoking Cessation
How does tobacco affect my oral health?
All types of tobacco – including cigarettes, cigars and chewing (or smokeless) tobacco – are harmful for your oral and overall health. In addition to containing nicotine, which is highly addictive, tobacco can increase your risk of:
- oral cancer
- periodontal (gum) disease—a leading cause of tooth loss and sensitivity
- delayed healing after a tooth extraction or other oral surgery
- fewer options for some kinds of dental care (smokers can be poor candidates for particular treatments such as implants)
- bad breath
- stained teeth and tongue
- diminished sense of taste and smell
How can tobacco cause periodontal (gum) disease?
Smoking may be responsible for almost 75 percent of periodontal diseases among adults. Tobacco products damage your gum tissue by affecting the attachment of bone and soft tissue to your teeth. An example of the effect is receding gums. A receding gum line exposes the tooth roots and increases your risk of developing a sensitivity to hot and cold, or tooth decay in these unprotected areas.
What effects can smokeless tobacco have on my oral health?
Like cigarettes, smokeless tobacco products contain a variety of toxins associated with cancer. At least 28 cancer-causing chemicals have been identified in smokeless tobacco products.
Smokeless tobacco is known to cause cancers of the mouth, lip, tongue and pancreas. Users also may be at risk for cancer of the voice box, esophagus, colon and bladder, because they swallow some of the toxins in the juice created by using smokeless tobacco.
Smokeless tobacco can irritate your gum tissue, causing periodontal (gum) disease. Sugar is often added to enhance the flavor of smokeless tobacco, increasing the risk for tooth decay. Smokeless tobacco also typically contains sand and grit, which can wear down your teeth.
Tips on quitting
Four in 10 smokers make an attempt to quit during the course of a year, but the withdrawal symptoms of nicotine are so severe, most smokers fail on their first attempt – less than two percent manage to remain smoke-free a year after quitting.
Deciding to stop smoking is the best decision you can make for your health, but it is also one of the hardest feats to accomplish.
- Set a date in the near future. This will allow you time to prepare yourself mentally and emotionally. Choose a time when stress will be lower.
- Tell your family, friends and co-workers that you are quitting. Building a support system will improve your chances of quitting.
- Investigate and use all resources available to you, such as books, websites and brochures
- Tell your dentist or physician you are quitting. Not only can they provide guidance and support, they can recommend and prescribe tobacco cessation medication.
- Avoid environments or situations that could tempt you, or put you in contact with people who smoke.
- Anticipate triggers to tobacco use and be prepared to avoid them. Chew sugarless gum, go for a walk or pick up a hobby to distract you.
- Reward yourself for reaching small goals. For example, treat yourself to a nice meal with family or friends to celebrate one week of being smoke-free.
- Put the money you would normally spend on tobacco in a jar. At the end of the year, take that money and spend it on a vacation or a new wardrobe!
Fluoride (Anti-cavity) and Tooth Sensitivity Treatments
Fluoride is a mineral that occurs naturally in many foods and water. Every day, minerals are added to and lost from a tooth’s enamel layer through two processes, demineralization and remineralization. Minerals are lost (demineralization) from a tooth’s enamel layer when acids — formed from plaque bacteria and sugars in the mouth — attack the enamel. Minerals such as fluoride, calcium, and phosphate are redeposited (remineralization) to the enamel layer from the foods and waters consumed. Too much demineralization without enough remineralization to repair the enamel layer leads to tooth decay and often, to tooth sensitivity.
Fluoride helps prevent tooth decay and sensitivity by making the tooth more resistant to acid attacks from plaque bacteria and sugars in the mouth. It also reverses early decay. In children under six years of age, fluoride becomes incorporated into the development of permanent teeth, making it difficult for acids to demineralize the teeth. Fluoride also helps speed remineralization as well as disrupts acid production in already erupted teeth of both children and adults.
Tooth sensitivity can also occur due to gum recession, aggressive tooth brushing, clenching and grinding (bruxism), weak or missing enamel, and deep restorations. Fluoride varnish applied at your visit or prescription strength fluoride toothpaste can help reduce or eliminate tooth sensitivity as well as tooth decay. You may also benefit by having a Desensitization Treatment, which is another way to treat your sensitivity. We can help determine which may be your best option for tooth sensitivity treatments.
Please Contact us to book your Appointment.
